Endometrial cancer
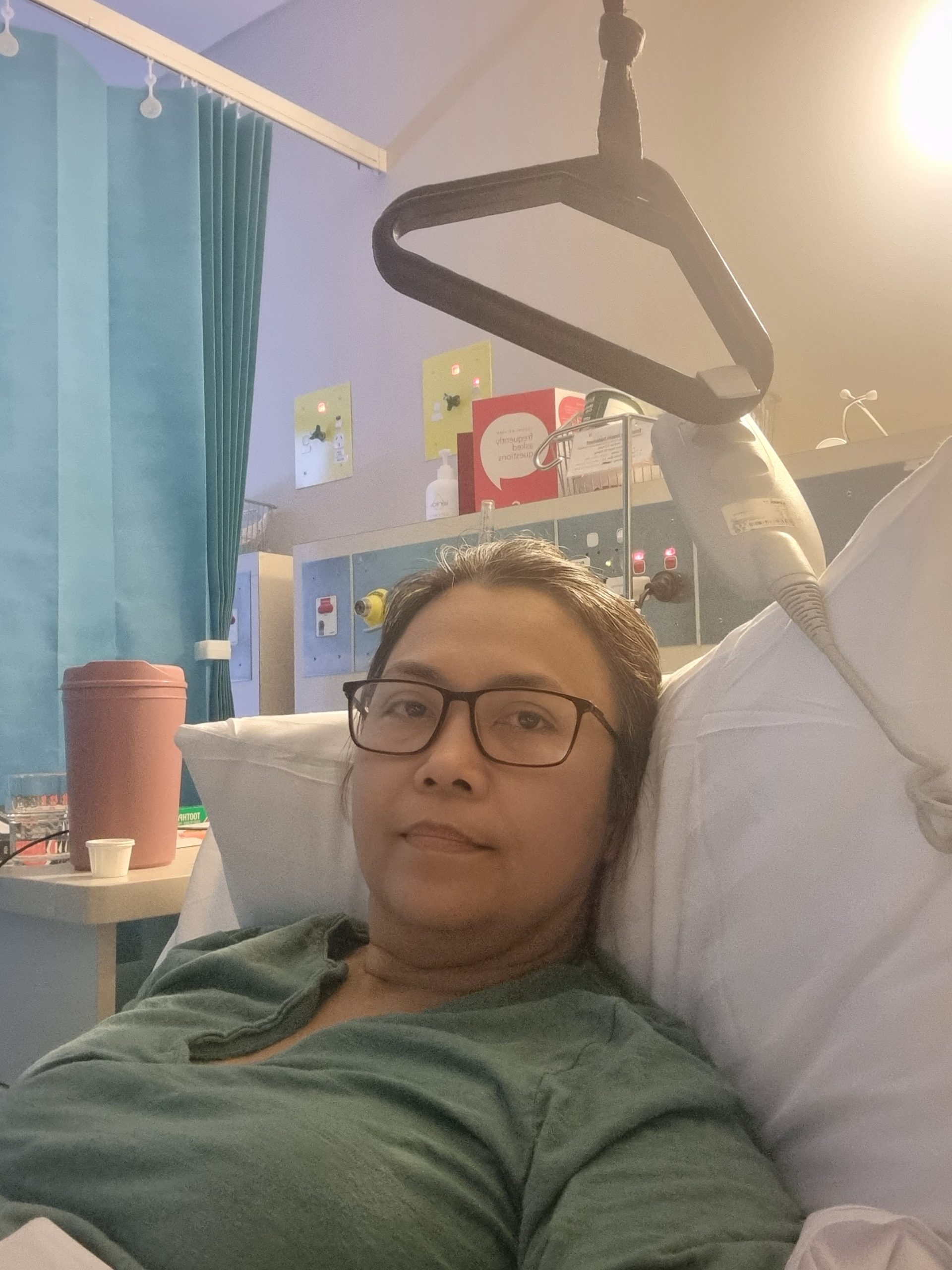
Mary facing the fight of her life.
My unexpected “call to adventure”
I received my “call to adventure” 17 days into 2023 when my Gynaecological Oncologist/Gynaecologist uttered the three words, “You have cancer.”
These three words suddenly altered my reality, a detour from the life I know.
Initially, I could not bring myself to utter the 6-letter word. I chose to label it the “Cheeky C”. I could not believe that my body took a genetic wrong turn, and the “Cheeky C” opted for my body as its playground.
Taking a break from LinkedIn and other social media platforms was helpful, as I turned inwards to make sense of this new reality. The diagnosis affected not only me, the patient, but my significant other, family, friends, colleagues – the whole community. I found our household entering a new physical, emotional, and social journey.
Family and friends have asked how I felt during the initial weeks. All I could say was there was a lot going on between Ms Chimpy (my emotional brain) and Rational Mary.
I was briefed that the endometrium, the lining in my uterus or womb, had thickened. Never once expecting to be saving the webpage of the Cancer Council on my browser as a favourite, I grew increasingly grateful for well-researched and helpful content for reference, as I navigate this new terrain.
Uterine cancer is the tenth most diagnosed cancer in Australia, and it is estimated that one in 44 females will be diagnosed by the time they are 85. I am one of the 44 females. A friend reminded me that I am more than a statistic. I am grateful to her for the reminder.
All along, I have enjoyed great health. This diagnosis was totally out of the blue for me. As there was no family history of this cancer, everyone was equally shocked with my diagnosis.
At any stage after a cancer diagnosis, like many cancer patients, I experienced times of distress and felt a range of strong emotions, such as disbelief, fear, anxiety, anger, and sadness. I could easily relate to the Kubler-Ross Change Curve (or also Kubler-Ross Model).
Leaning on the medical team and the people around me to navigate through this new reality was imperative. I chose to lean onto my doctors and a team of health professionals, minimise disruption, increase healing vibes, and be 100% focussed on coming out strong on the other side. I was determined to own my story of mind over matter, with the faith that the universe has my back!
At post-menopausal, my diagnosis appeared to be random, as I had not experienced any symptoms of endometrial cancer prior. For example, I had none of these symptoms:
- bleeding after been through menopause
- unusually heavy periods and bleeding in between periods
- any unusual fluid or discharge
- pain in the belly or abdomen
- trouble going to the toilet to pass urine (wee) or pain.
I am always grateful to my general practitioner (GP) for taking my one-off blood clot seriously. My GP figured that it was best for me to undergo further investigation. She was undeterred by how close to Christmas we were. She issued referral letters to multiple Gynaecological Oncologist/Gynaecologist across Melbourne, to ensure I secured an appointment soonest possible to be seen by a specialist.
When endometrial cancer is discovered at an early stage of its development in the body, most women are cured. Even if the disease is not discovered until after it has advanced, treatment is still possible, but the likelihood of a long-term cure is lower.
Legally, I have the right to my privacy and may choose not to disclose what I went through. However, I am choosing to be open about my condition for a few reasons:
- I want to reduce stigma for people if they ever feel they cannot share when faced with unexpected life events.
- In working with business leaders, managers, employees, and clients, I have witnessed how exhausting it can be for those who chose to keep their condition or difficult personal situations a secret. Keeping challenging life altering conditions to yourself is depleting and fatiguing. Conserving energy for healing and recovery is life changing.
- I was determined to find a way that works for me, to ensure my emotional health needs are met, so that I am set up in a better position to manage the demands of treatment.
- To remind all of us not to take our health for granted by paying attention to what our bodies are telling or not telling us.
- I want to embody the change I want to see in women being responsible for their bodies.
- I cannot emphasize enough the benefits of establishing a strong relationship with your GP.
Reasons to have your own General Practitioner (GP)
A GP who knows you and your medical history
Visiting the same GP regularly will ensure you are seeing a medical professional who knows you and your medical history. Over time, you can build a relationship with your GP. A strong relationship with your GP will help to ensure you are getting care and treatment from someone you trust. Establishing an ongoing relationship with a GP is a lifelong investment for you and your family’s health.
Preventative and general health advice from an expert
A regular GP is trained to assess, treat, and advise you on various physical and mental health symptoms. Moreover, they will usually be the first point of contact for most health issues throughout your life. They don’t just treat coughs and colds – they’re among the best resources for providing science-based information for preventative care and living a healthy lifestyle.
I will always be grateful to my GP, for taking the one-off blood clot episode seriously.
Chronic medical conditions
GP’s can help you manage a range of chronic medical conditions. A GP can also complete a Health Care Management plan specific to your needs and requirements. This makes them an important contact for accessing resources and other services that may be useful for managing your medical conditions.
Referrals and coordinated care
Your GP has connections to other health professionals if your conditions require specialised treatment. They can connect you with specialist doctors, and other primary healthcare services, including, women’s doctors, psychologists, physiotherapists, and podiatrists.
Looking back, my adventure seems unreal — like a dream that happened to someone else, and I am glad of early detection and swift medical intervention. I am proud for making it through, and above all, to be cancer-free.
Mary turned to art therapy to help her through her recovery.
Who we are
We are the Australian Gynaecological Cancer Foundation. The only organisation that focuses on funding laboratory research into all eight gynae cancers.
Subscribe to our newsletter
Get in touch
Where to find us:
1/1 Jamison Street, Sydney NSW 2001
For general enquiries:
telephone: +61 2 8235 2606
email: info@agcf.org.au
Together, we’re giving women hope.
Donations of $2 or more are tax deductable in Australia.
ABN: 17 152 685 295

© Australian Gynaecological Cancer Foundation | Privacy Policy